 [Episode 14] In today's podcast, we're going to talk about the therapies that take a cognitive-behavioral approach to working with people. I review the theoretical assumptions, therapeutic process, techniques, use in culturally competent practice, and strengths and limitations of CBT. This podcast is longer than most because I use a lot of clinical examples and dialogue to illustrate the concepts. [Pictured: Tim Beck, developer of CBT, and Albert Ellis, develop of REBT]
[Episode 14] In today's podcast, we're going to talk about the therapies that take a cognitive-behavioral approach to working with people. I review the theoretical assumptions, therapeutic process, techniques, use in culturally competent practice, and strengths and limitations of CBT. This podcast is longer than most because I use a lot of clinical examples and dialogue to illustrate the concepts. [Pictured: Tim Beck, developer of CBT, and Albert Ellis, develop of REBT]
Download MP3 [47:11]
A partial list of cognitive distortions can be found at Wikipedia: http://en.wikipedia.org/wiki/Cognitive_distortion
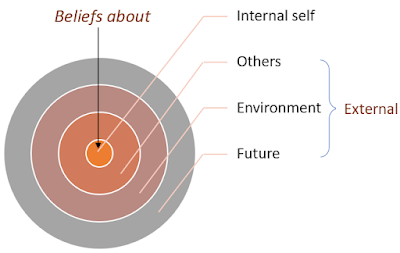
This figure illustrates levels of thinking, from external to internal. The downward arrow technique moves the client from external beliefs about the future, the world and others, to internal beliefs about themselves. This is a key construct in cognitive therapy. You can see the influence of psychodynamic theory, with the focus of attention moving inward. The practical application of this model, however, focuses on what the patient can understand about themself without the need for someone else to interpret their world. This makes CBT very different than in psychodynamic.
Transcript: Cognitive Behavioral Therapy
Jonathan Singer: Hello and welcome. You have found the social work podcast. My name is Jonathan Singer and I’ll be your host as we explore all things social work.
In today’s podcast, I’m going to be talking about Cognitive-Behavioral Therapy, or as it is often referred to as CBT. CBT is a relatively new kid on the psychotherapy block. If we think about the neighborhood, we can say that Freud lives in the old and somewhat creaky mansion on the hill; B.F. Skinner, known to the folks in the neighborhood simply as Burrhus, lives in a very functional, if somewhat boxy condo. Down the road you’ll find Carl Rogers; although, not primarily known as a decorator, Rogers has an uncanny ability to take his vision of what his house should be like and match it with what his house actually is. As a result, Rogers’ place is a genuinely cozy and authentic house. And although Freud, Skinner and Rogers don’t usually agree on much, they routinely get together and complain to the neighborhood association about the ‘in your face’ appearance of Fritz Perls house. The existentialists, Yalom and May - they are more likely to rent than to own. After all, who knows what life will bring, right? But because they are regularly consulted by others during renovations, their influence can be felt in almost every house on the block. This brings us to the new kids on the block. The Cognitive-Behavioral therapists like Albert Ellis, Aaron Beck, Donald Meichenbaum, and Michael Mahoney. They grew up in this neighborhood. Ellis and Beck followed Rogers’ footsteps and moved out of Freud’s house when they were young and set up their own places. Meichenbaum and Mahoney, on the other hand, they were staying with Skinner. What we now call CBT grew out of both the psychoanalytic and the behavioral houses. In future podcasts, we’ll talk more about the other inhabitants of this psychotherapy neighborhood, including: William Glasser, Insoo Kim Berg and others.
The Theoretical Neighborhood (click to enlarge)
This visual of the "theoretical neighborhood" I described in the introduction to the podcast was created by MSW students in Claudia Dewane's Clinical Practice I course at Temple University Harrisburg. Thank you!
Today, however, we will focus on CBT, the theoretical assumptions, the therapeutic processes, techniques, use in cultural competent practice and strengths and limitations. Before we start though, I want to make it clear that CBT is not a single therapeutic approach. CBT is a collection of therapies that place differing amounts of emphasis on the roles of cognitions, emotions, behaviors and the roles that they play in our happiness. Some like Albert Ellis’ rational emotive behavior therapy or REBT assumes that there is an objective reality that can be distorted. Others like Mahoney’s cognitive constructivism assume that reality is socially constructed. The REBT therapists can safely argue that someone’s thoughts are rational because the assumption is that some thoughts are rational and some are not, are all based on an objective reality. Now, although the constructivists would contend that mental processes are central to understanding the human condition, they would never say that what we thought could be objectively more rational than another. Yet these are two therapies that fall under the category of cognitive behavioral. So, if someone says, ‘Yeah, I do CBT’ ask them for more specifics.
Theoretical Assumptions: The most basic assumption of CBT is if you want to change the way you feel and the way you behave, you have to change your thinking. As Vonk and Early (2009) write in their excellent summary of CBT in the Social Workers’ Desk Reference: “Psychological distress is largely a function of disturbances in cognitive processes.” CBT assumes that negative and unrealistic thinking give rise to emotional disorders. Altering our cognitive processes can reduce emotional disorders and increase our functioning; however, research also supports the idea that our thoughts are influenced by our emotions and behaviors. For example, the physical act of smiling improves mood, that is, behavior influences mood. Arthur Freeman and his colleagues, in their text, Clinical Application of Cognitive Therapy cite research that found that sadness facilitated the recall of sad events, whereas happiness facilitated the recall of happy events. These are examples of mood affecting how we access cognitions, and of course, multiple times a day we choose to behave certain ways based on our thoughts.
So, another assumption of CBT is that there is a reciprocal relationship among cognitions, emotions, and behaviors. Imagine you’re working with a woman whose daughter died in a car accident. We’ll call her Isabella. What is the relationship between Isabella’s thoughts, feelings and actions? Freeman and his colleagues suggested that this reciprocal relationship can turn into a self-perpetuating cycle. So, let’s say that Isabella had a biological predisposition to depression. The external event, her child dying in a car accident, triggered a depressive episode. Let’s say that Isabella also had a core belief that she is unworthy of happiness. In this situation, her core beliefs, mixed with the external events triggering automatic thoughts such as: ‘this was my fault’, ‘I should have kept her at home’, and ‘I don’t deserve to live’. These automatic thoughts influence her emotional response, sadness and hopelessness. They also influence how she behaves around other people. For the sake of simplicity, let’s say that Isabella withdraws from social situations. Her behavior then influences the way others respond to her. They might stop calling, talking to her and these responses then influence her automatic thoughts. At the same time, these automatic thoughts triggered the feelings of sadness. As I mentioned before, sad feelings facilitate the recall of unhappy events. So, her sadness makes it easier to remember the unhappy experiences in her life, providing her with further evidence (however biased it may be) that support her thoughts and feelings that things are hopeless. This example illustrates the reciprocal influence of thoughts, feelings and actions and how psychopathology can be perpetuated by this cycle.
The therapeutic process can intervene at any point in this cycle, that’s why CBT has interventions that address behaviors and emotions, as well as cognitive processes. Now, the therapeutic process in CBT has to do with the goals of treatment, the relationship between the client and the therapist, as well as the particulars of assessment and intervention. Regardless of the particular variant of CBT, the goals of treatment share the following elements: identifying cognitive content, examining cognitions to determine their effects in emotions and behaviors and developing interventions to help clients utilize alternative and more adaptive cognitions.
[7:20] Also common to all CBTs is that these elements can be applied in an individual, family or group setting. Albert Ellis states that two of the main goals of rational emotive behavior therapy are: to assist clines in the process of achieving unconditional self-acceptance and of others, and to see how the two are inter-related. The assumption is that as clients start to accept themselves, they will be better able to accept others. Now, Ellis assumes that although people have the potential for happiness, that we are also fallible. Because we are fallible, Ellis believes that a goal of therapy is to help people accept themselves as they are, fallible creatures who will make mistakes, but at the same time, have the potential to learn and grow from those mistakes. Ellis illustrated this idea very clearly in the now classic therapy session with Gloria. Gloria says she doesn’t want to be an ordinary Jane Doe. Ellis challenges her to consider what would be so awful about being an ordinary Jane Doe. He is not saying she should settle for mediocrity or have no sense of achievement, rather he’s addressing a core belief that ‘if my life isn’t special or unique, then it’s awful’. In Beck’s cognitive therapy, schemata, also known as core beliefs, are the targets of interventions. So, a basic goal of cognitive therapy is to change the way clients think, using their automatic thoughts to reach their core beliefs or schemata and begin to restructure how they understand the world.
Depending on the variant of CBT, the role of the therapist and the client is more didactic, that is, teacher/student focused or more collaborative, for all CBT treatment is seen as an educational process. The therapist is seen as an expert in cognitive behavioral methods, someone who actively teaches or coaches the client about automatic thoughts, core beliefs, and ways to restructure thinking, as well as someone who gives homework. The CBT practitioner strives to be as transparent as possible. What I mean by transparent is that if the practitioner recognizes an automatic thought, she will say to her client, “I just heard you express what I call an automatic thought”. The practitioner would then go on to define the term, give examples of what an automatic thought looks like and tell the client how they can do just what the therapist did. In REBT, Gerry Corey (2005) notes that clients learn three things; the first is to identify and dispute irrational beliefs that are maintained by self-indoctrination; Second, to replace ineffective ways of thinking with effective and rational thoughts; and finally, to stop absolutist thinking, blaming, and repeating false beliefs. In contrast, Beck sees the client/therapist relationship as being most successful when there is empathy, genuineness, and unconditional positive regard. Now if these qualities sound familiar, it’s because they are associated with Carl Rogers, you know, the guy that lives down the block. Unlike Rogers, however, Beck believes that although these qualities are necessary for therapeutic exchange, they’re not sufficient to produce optimum therapeutic effect.
In CBT, as with all other forms of treatment, the therapeutic process starts with an assessment. I review the basic components of assessments: bio, psycho, social spiritual, mental status exam, and diagnostic statistical manual for social workers in podcasts that can be found on socialworkpodcast.com. The unique contribution of the CBT assessment is what Vonk and Early call the cognitive analysis. Although the analysis can take many forms, it essentially identifies the problems, thoughts, feelings and actions that accompany those problems. Then a working hypothesis is developed to explain the relationship between the specific problem and the client’s unique responses. In REBT, the cognitive analysis uses the ABC technique. In this approach, the therapist looks for an ABC pattern where: A is the activating event (for example, a child is killed in a car accident), B is the belief (now that she’s dead everything will be awful) and C is the resultant emotional and behavioral consequences (such as sadness, fear and isolating behaviors). Notice how the belief comes in-between or mediates the relationship between the event and the feelings and behaviors. That’s because CBT assumes that events do not cause feelings and behaviors, rather our views of those events, or interpretations of those events, are what causes our feelings and behaviors. This assessment allows the therapist to identify consistent and predictable patterns of behavior that can then become the target of intervention. The ABC assessment has a corresponding D, E and F intervention and outcome component that we’ll talk about later on in the podcast.
Before we move on to techniques and interventions, I’d like to talk briefly about the structure of a cognitive therapy session. Because CBT is a time-limited treatment, and it addresses a few issues, CBT therapy sessions need to be focused and productive. To that end, Freeman and his colleagues describe one way to structure a CBT session. First, the session begins with agenda setting. This is a collaborative process wherein the client and the therapist can be sure to cover topics that are relevant and central to treatment. This does not prevent flexibility during the session, but it makes it easier for the CBT therapist to redirect and avoid what is known as door knob comments. The door knob comment refers to a situation where a client brings up a significant issue on his way out of the door. Imagine your client with his hand on the door knob say, “Oh, by the way, my mom tried to kill herself last night and I’m heading to the hospital to see her”. Why clients do this is up for debate. One commonly suggested reason is that it is a chance to unload burdensome topics without having to address them. But regardless of the reason, setting an agenda helps to identify what issues are most important at the beginning of the session and to decide what topics will be focused on during the course of the session.
Number two, after the agenda has been set, you review your client’s current status, including what has transpired between sessions. For example, if we think of the mom whose daughter was killed in a car accident, it would be useful to know if there were any deaths of any close personal friends or related events to the death of her daughter among other things, in the past week. This quick check also sets the tone for the session and allows the client the opportunity to focus on being present in the session.
The next step is to ask for feedback. Now feedback can either be about the previous session, or if you ask about feedback at the end of the session, it can be about the current session. Although Freeman and his colleagues suggest that this is an optional step, my experience has been that regular feedback is invaluable to addressing interpersonal issues that clients might be unwilling or uncomfortable to share otherwise. For example, if during the beginning of a session, I ask my client if he thought that what we talked about during the previous session helped him during the week and he said no, then I would have the opportunity to explore what we could do differently. It could be that all he could remember about the session was me being confrontational. And obviously, this information is crucial to addressing how I approach him, how I approach the therapy, so that we can have a successful outcome.
The fourth step is to review the previous week’s homework. Because CBT believes that most change occurs outside of the office, homework is an integral part of treatment; however, homework will not be successful if you’re not clear about the relationship between homework and your client’s goals. It is the classic story of Albert Ellis and the homework he assigned himself one summer. According to Gerry Corey (2005), Ellis was thinking of ways to overcome his shyness around women. He decided he would speak to 100 women over a period of one month. Although the conversations did not result in a date, the story goes that he did de-sensitize himself to the fear of rejection. This story clearly illustrates the value of making a direct connection between the client’s goals and the work they do outside the session. Imagine telling a client with social phobia that they should talk with 100 strangers. Unless you’re very clear as to why this activity is the best for your client to solve their problems, they’re likely to look at you and laugh, or more realistically, they are more likely to agree with you and then just not do it. Freeman and his colleagues (2004) suggest a brilliant way of introducing the idea of homework to clients on page 29 of their text. They suggest saying something like, “One of the things I like to do is to think in terms of what the people I work with can do between sessions to get results more quickly. How does that sound to you? Do you have any ideas what would be useful to do between now and the next time we meet?”
Covering these first four items doesn’t need to take more than 10 minutes. The remainder of the session can be spent on addressing the last sections of a therapy session, which include: the main agenda items and developing new homework.
REVIEW
So, before I move on to the really fun stuff, the intervention techniques, I want to quickly review what we’ve gone over so far. CBT is an umbrella term that applies to the therapies that assume that behaviors and emotions are influenced by our cognitions. The basic goal of CBT is to identify and replace dysfunctional thoughts with functional thoughts in order to improve mood and develop healthy behaviors. This process is collaborative and expects the client to participate actively during treatment, inside and outside the therapy session. Now we’re going to take a short break, but when we come back we’re going to talk about some of the techniques used in CBT, the use of CBT in culturally competent practice and the strengths and limitations on the use of CBT in social work practice.
[18:10] Music Interlude: QuinTango performing “Por una cabeza” http://www.amazon.com/Por-una-Cabeza/dp/B000SGU4M0
Welcome back. We are going to continue our discussion of cognitive behavioral therapy by turning our attention now to the techniques and interventions.
Techniques and Interventions: Because cognitive-behavioral therapies believe in a reciprocal relationship between cognitions, emotions and behaviors, CBT uses techniques that address how we think, feel, and act. Today, we are going to focus our attention on the cognitive, and to a lesser extent, the emotive techniques. For a review of behavioral techniques, you can listen to the behavior therapy podcast at http://socialworkpodcast.blogspot.com/2007/03/behavior-therapy.html. The cognitive techniques developed by Ellis, Beck, Meichenbaum and others are widely used by therapist that do not consider themselves strict cognitive behavioral therapists. Corey notes that rational emotive behavior therapy was really the first cognitive behavioral therapy. The name rational emotive behavior therapy tells you right off the bat that REBT distinguishes between rational and irrational thoughts, but also focuses on feelings and actions. The assumption is that irrational ideas lead to self-defeating behavior. Corey (2005) gives some examples of irrational ideas: ‘I must have love or approval from all of the significant people in my life’, I must perform important tasks competently and perfectly’, ‘if I don’t get what I want, it’s terrible and I can’t stand it’. Now, as a side comment, Ellis is known for using humor to help his clients recognize irrational thinking. In fact, use of humor is one of his techniques. For example, he called irrational thoughts “I must” mustabatory thinking and he would caution his clients against musterbating. One technique Ellis uses in intervening with irrational thinking is called disputation. The way it works is that once an irrational idea has been identified, Ellis will dispute that idea until clients no longer believe the idea, or at the very least, do not believe it so strongly. For example, if your client irrationally believes that any conflict is bad, Ellis might say, “Can you think of a circumstance when conflict is good”? If they can think of a single instance, then Ellis would say that the belief, as a general rule, is clearly false. The client would then figure out a belief that was a rational one, such as, some conflict is counter-productive.
Remember earlier in the podcast, I talked about the ABC model where A was the activating event, B was the mediating belief, and C was the resultant emotional and behavioral consequences? Well the last 3 steps in the model are cleverly called: D, E and F. The D stands for a disputing intervention. Disputation targets the belief in the way we have just talked about. The disputation has the effect or E. The E is that the more effective or functional philosophy is developed. For example, if we think about our client, Isabella, whose daughter died in a car accident, the disputation might help her change her belief from ‘everything is awful’ to ‘I wish some things were different’. This E or effect, results in a different feeling or F, like hope. This is how you get ABCDEF as an intervention that can be used to address cognitions, behaviors and feelings. Another technique that Ellis uses to address irrational thinking is changing the language that clients use. If your client says, “I should do this” or “I should do that”, Ellis would say that they are shoulding on themselves. Don’t should I me, I won’t should on you. When we believe we should do something, we confuse preference with needs. The statement: “I would prefer to fold laundry before bed” is a very different message than “I should fold laundry before bed”. Although subtle, the technique is congruent with CBT theory. As Lakoff and Johnson illustrated in their text, Metaphors We Live By, our words both reflect and create the world we live in. If we can change our words, then we can change the way we think, feel, and act. Aaron Beck believes that words are important, but he’s more interested in listening to words to identify schemas, automatic thoughts and cognitive distortions.
Beck conceptualizes problematic beliefs and thoughts not in terms of what is rational or irrational, because that’s up for interpretation. But instead, beliefs are problematic when they are too rigid, too absolute, too broad or too extreme. In Beck’s version of CBT, people develop unconditional core beliefs, also known as schemas, which influence feelings and behaviors. Unconditional core beliefs are beliefs that are too rigid, absolute, broad or extreme. For example, if I have a core belief that I am a fake, it means that my core belief is that I’m always a fake, not that I’m sometimes, or in some situations, or to some degree. Beck believes that these qualifiers do not apply to dysfunctional core beliefs. The truth is that sometimes I am a fake, but that’s not what the core belief says. No, the unconditional core belief is that I am always a fake. This is clearly not true, and I can point to at least 3 times in my life when I have not been a fake. Sure, they were all back in the 1980’sm but nevertheless, they’re exceptions. If I had a laugh track, I’d be playing it right now, but I don’t. Note to self, get a laugh track.
So, if we are not aware of our core beliefs, how do we identify them? Beck suggests that we can get to core beliefs by identifying automatic thoughts. Freeman and colleagues define automatic thoughts as: ‘spontaneous cognitions in reaction to stimulus that leads to emotional responses”. For example, you get a test back and you see that you got an F. Your automatic thought might be that I’m going to fail the class. Now, you might not be aware that you had the thought, but you’re probably going to be aware of the feeling that follows. It could be fear, sadness, or anger. Or it could be relief and happiness. Now, if it is relief and happiness, this is just another piece of supporting evidence that cognitive behavioral therapy has some validity. For example, your thought might be ‘I hate this class and the only excuse I would have for dropping it is if I fail the first test’. Then I would feel relief or happiness when I see the failing grade. So, it’s not the grade that creates the feeling, but rather the intervening belief that informs how I will feel about something. So, the way to get to core beliefs is through automatic thoughts. It’s not enough to change my automatic thoughts though. In order to really change, I have to address my core beliefs. Greenberg and Padesky liken core beliefs and automatic thoughts to weeds in a garden. The automatic thoughts are the weeds and the core beliefs are the roots. If you want to get rid of the weeds once and for all, you have to dig up the roots. So, it’s not enough to get out the weed whacker and go to town. If you cut off the tops of the weeds, they’ll just grow back again. Likewise, if you don’t deal with the core beliefs, your automatic thoughts will just keep coming back.
One technique that Beck uses to identify the core beliefs is called the downward arrow technique. The way it works is that your client identifies a situation, doesn’t have to be a big deal situation, it could be anything where she had an emotional response. The good news about these core beliefs is that they establish predictable patterns so you are able to access core beliefs using a variety of situations. They don’t have to be intense, the most painful or the most significant ones. They could be something minor like ‘yeah, this guy yelled at me today’ or ‘I realize I showed up for work 15 minutes late’. The downward arrow moves from the situation you’re most aware of, which is the event, to uncovering the automatic thoughts, some of which you may be aware of and some you may not be aware of, and then ultimately uncovering the core belief.
[27:30] The following dialogue is an example of the downward arrow technique.
T: When Bob said he was too busy at work to have dinner with you, what went through your mind?
C: That he doesn’t want to be with me.
(Ok, so when he says ‘he doesn’t want to be with me’, that’s an automatic thought. Notice that it is external, it’s about somebody else).
T: If that were true, that he doesn’t want to be with you, what would that mean?
C: That he doesn’t care enough.
(So, in this one we move from his choice to statement about this person).
T: And what would that mean?
C: If he doesn’t love me, no one will.
(And now we’re moving deeper. He doesn’t really love me, we move deeper into his perception of his own core experience. We are getting closer to the core belief).
T: And if it were true, that he didn’t care enough, what would that mean?
C: That he doesn’t really love me.
(Ok, now he says, ‘if he doesn’t love me know one will’, this moves to the internal. This is about my client).
T: And what would that mean?
C: I’m unlovable.
(And finally we get to the core belief. This is my client’s core belief about himself).
T: And what would that mean?
C: Just that, I’m unlovable. No one will love me.
(Now if you noticed, he repeated that nobody else will love me. When you get repetition, it means you have hit bottom, that this is the client’s actual core belief).
Using the phrase ‘what does that mean’ can get a little old. So, some variations include: ‘If that’s true, what’s so bad about…’? Or, so, what’s the worst part about…’? Or, ‘so, what if…’ or ‘what does that mean about you’? Beck recognizes that we perceive situations correctly, but because of dysfunctional beliefs, we can draw erroneous conclusions. The process that results in correct perceptions leading to erroneous conclusions is called cognitive distortion. Everyone has cognitive distortions, not just people with diagnosable mental illnesses. In his 1999 revised edition of “Feeling Good: The New Mood Therapy,” Burns identifies commonly observed cognitive distortions. One cognitive distortion is called dichotomous or ‘all or nothing’ thinking. In this cognitive distortion, things are seen in mutually exclusive categories. All good or all bad. For example, I was seeing a couple for couples counseling and the boyfriend was having problems with his girlfriend. Obviously, or they wouldn’t have been in couple counseling. But we were talking about a specific situation, and my client said that during the situation his girlfriend was mad at him. And because we were in a couple counseling situation, I could turn to the girlfriend and ask her, ‘Is it true? Were you mad at him?’ And she said yes. So, my client correctly perceived that his girlfriend was mad at him in that situation. But, because he employed the cognitive distortion of ‘all or nothing’ thinking, he erroneously concluded that she was basically a mean person. Once we identified the cognitive distortion, then we were able to move on from there and intervene appropriately, recognizing where the client had gone wrong in his thinking. Another type of cognitive distortion that Burns talks about is called mindreading. If your client is employing the cognitive distortion of mindreading, they are thinking that they know what somebody else is thinking, without any supporting evidence.
I saw this cognitive distortion all the time when I was working with kids in school settings. For example, I was working with this 13 year old called Manuel, who was suspended for fighting. When I asked him what happened, he said, “Raymond was looking at me disrespectfully”. When I asked him what made him think that the other kid was disrespectful, my client said, “Well, every time I look up, Raymond is looking at me”. So, this was an example of mindreading because Manuel assumed that he knew what Raymond was thinking. And, in fact, that Raymond was thinking disrespectful thoughts. The result of this cognitive distortion was a maladaptive emotional response. Manuel went from being annoyed to uncomfortable, irritated and enraged. This faulty expectation about how Raymond should act resulted in appropriate behavior on the part of Manuel. Specifically, Manuel decided that he couldn’t stand for this disrespect, so he waited until after school and he jumped Raymond. It was really no surprise to Manuel, or to me, that he got suspended for jumping another student after school. So, what do you do with this kind of situation? Well, cognitive-behavioral therapy supports the idea that you can intervene at the cognitive, affective or behavioral points in this scenario. And they are all congruent with cognitive behavioral therapy. So, a cognitive intervention might start with a supportive statement like, ‘It sounds like you think Raymond was dissing you’? If you are using rational emotive behavior therapy perspective, you might decide to challenge the irrational belief by saying, “I wonder what else might explain him looking at you’? Or, ‘I wonder what Raymond thought when he saw you looking at him’?
If disputation doesn’t work because of a lack of rapport or the client gets angry or frustrated easily, you could take Beck’s approach and see what thoughts, what pathways, to core beliefs exist. You might use the downward arrow technique and ask, “So, what’s the worst thing that could happen if it were true that Raymond was dissing you? Or what does it say about you if someone is being disrespectful?” An intervention to help emotions might be to use a feeling thermometer. The idea is to help Manuel identify his feelings and intervene before they escalate to the point of no return. And in Manuel’s case, the point of no return was rage. So, the way that it works is that you would take the feeling thermometer, which is essentially a piece of paper with a thermometer drawn on it and say, ‘The bottom is when you feel cool. The top is when you feel hot. Just like a real thermometer.’ Then you would ask Manuel to mark on the thermometer where he would place his feelings of being annoyed, escalating to being uncomfortable and then to angry and finally to being enraged. So then you would talk about what things he could do to keep the thermometer from rising. For example, when you feel annoyed, what sort of things would you be able to do different?
Finally, you could use the behavioral interventions to identify alternate to jumping Raymond, including: talking with a teacher or the school social worker, possibly waiting 24 hours before acting on his impulses, or having him play detective and have him keep track of the number of times Raymond is looking at him, when he looks at Raymond. You could also set up a mediated meeting between Manuel and Raymond to talk about the situation. In this way, you can address the emotional, the behavioral and the cognitive by having Raymond respond to the accusation, ‘you’re being disrespectful’.
So, what do you do when these cognitive techniques don’t work? Michael Mahoney in his 2003 text, “Constructive Psychotherapy: A Practical Guide” noted that cognitive methods worked best when people were willing and able to be aware of their self-talk. If cognitive therapy doesn’t seem to be working, that is, the client is unable to detach from the content and the emotions associated with the situation long enough to identify or acknowledge cognitive distortions, then it is reasonable to step down to basic behavioral interventions. If Manuel and I were talking soon after the incident with Raymond, it might be unreasonable to expect an angry 14 years old to respond well to strictly cognitive interventions. The best choice might be to start with the behavioral intervention with the intention of moving to a cognitive intervention later on.
Now, there are a number of other techniques used by cognitive behavioral therapists, including: problem-solving, assertion training, role-playing, and imaginal techniques, such as having your client imagine how she might think or feel in the best or worst of situations. Cognitive behavioral therapists have also developed a number of what I call paper and pencil interventions. These are often practiced in-sessions, but assigned as homework and commonly take the form of a sheet of paper where the client fills in information about events, beliefs, automatic thoughts, feelings, rational responses and alternate choices. Freeman and colleagues write about and include many examples of these types on interventions in their text, “Clinical Applications of Cognitive Therapy”. The interventions and techniques mentioned in this section are just the tip of the iceberg for what’s available through cognitive behavioral therapy.
If you are interested in learning more about interventions and techniques, I suggest doing a Google search or Amazon.com search on books having to do with cognitive behavioral therapy. I’m partial to the Freeman text. I feel that it’s a very practical and logical step-wise approach to working with folks. If you are working with folks that are suicidal, Rudd and colleagues (1999) published a book that deals with cognitive behavioral therapy and treatment and management of suicidal behaviors. And beyond that, there are cognitive behavioral treatment manuals for folks with obsessive compulsive disorder, panic attacks. David Barlow has an entire series of practitioners’ guides to treating a variety of different disorders. I think it’s from Guilford Press, but I could be wrong. I haven’t double checked that. So, the point is there are a lot of resources out there that you can find to learn about specific interventions or techniques for specific populations.
[38:20] As we move into the last part of this podcast, I’d like to talk about the use of CBT in culturally competent. Then end with some strengths and limitations of CBT, particularly with an eye towards its use in social work practice. Gerald Corey’s text, “Theory and Practice of Counseling and Psychotherapy” discusses some of the strengths and limitations of CBT in culturally competent practice. Corey notes that CBT has the advantage of spending the time to indentify a client’s core beliefs, rather than making assumptions of what people believe based on how they look or what neighborhoods they come from. The significant concern about mental health treatment is that multi-cultural populations tend to use less services that the majority White culture. And they tend to report lower rates of satisfaction with the services they do receive. CBT addresses these concerns somewhat by having treatment that is fairly structured and organized. This emphasizes practical solutions, increasing participation rates and overall satisfaction with services. In my own practice, I have found that CBT is useful in bridging cultural gaps because it’s connecting for my clients to know that irrational and distorted thoughts are experienced by everyone, from the most privileged and powerful to the most marginalized and dis-empowered. I have also found that it sometimes is easier for my culturally diverse clients to be honest about beliefs having to do with mistrust of dominant culture when using a CBT approach. As a White man, I want to know if my African-American teenage client believes that White people are not to be trusted. I also want to know if this belief is shared and supported by his community or if this is born of personal experience, or possibly both. Knowing the difference would influence how I would proceed in my treatment.
There are a number of limitations of CBT in culturally competent practice. The first is there is an emphasis on challenging clients’ beliefs and labeling thoughts as irrational and this can be perceived as an irresponsible use of power. For example, if my client came in and said that he didn’t trust White people and I called that an over-generalization, I could very quickly lose any existing rapport and probably paint a bad picture of what social workers are like and what therapy is. More importantly, however, I would be ignoring the social context that informed those cultural beliefs. A second limitation is that some of the techniques, such as challenging beliefs, might be in conflict with clients that have a group or family vs. individual orientation. As a privileged White male, I am expected to be an individual who could challenge others and be competitive to my own advantage. That might not be the case for many of my non-White clients. A final limitation is that the didactic or teaching orientation of CBT can set up an expectation that the therapist will solve the problems for the client, especially if the client comes from a culture where the opinions of professionals are held in high regard.
Now, the last part of this podcast is a look at the strengths of CBT and some of the limitations, particularly as far as social work is concerned. So, one of the strengths of CBT is the idea that events do not cause us to be happy or unhappy; Rather, it is our perception of the event. Clients become their own teachers in a CBT model. It’s an empirically validated treatment for depression, anxiety, phobias, obsessive compulsive disorder, eating disorders, and a number of other psychosocial disorders that we address in social work practice. And because of the large amount of information available, CBT is an accessible model of intervention for both novice and experienced practitioners. The emphasis tends to be on measurable outcomes and that makes it a lot easier to document and to be accountable, both to your clients and to the third party payers. Because it targets specific problems, CBT is usually short-term and that’s a characteristic desired by both clients and third party payers. Targeting specific problems enables treatment to be individualized. This is a core value of social work. It can be used with individuals, families and groups, something that social workers do all of. It supports the social work value of self-determination and the client’s active involvement is consistent with social work’s empowerment approach. Finally, the techniques are portable. Because social workers are often in the field with clients, we can implement CBT techniques in the here and now, regardless of the setting.
Some of the limitations include that: the focus is on problems rather than solutions. Another limitation is as we mentioned in terms of culturally competent practice, it can be confrontational and that can be off-putting or seen as culturally insensitive. Therapists can get caught up in technique over rapport and therapeutic alliance. Another limitation is the risk of imposing the therapist’s idea of what constitutes rational thinking. Another limitation is the critique or criticism that CBT is simply the power of positive thinking at work. Really, it’s not you environment, it’s not your neighborhood, it’s not policies that are causing you to be unhappy, it’s just because you’re thinking you’re unhappy. Think positively and you will be happy. Well, CBT is not that simplistic, but it can be a limitation if the therapist is not adequately trained and grounded in the theory and knowledge about how to incorporate the external with the internal. Another limitation is that CBT can minimize feelings, although doesn’t necessarily have to. CBT assumes an objective reality and we sort of alluded to this before, where we were talking about Mahoney’s constructivist theory, where the idea is that constructivists believe that we construct our own realities. Folks like Ellis state there is some kind of objective reality from which we can decide that something is rational or irrational. Now, to Ellis’ credit, he did say that essentially, I am a constructivist; although, I’m not really sure how that fits with his model. But nevertheless, the final limitation of cognitive behavioral therapy is that it assumes that the behavior will change if clients learn to act rationally. And as we all know, thinking rationally about something is no guarantee that behaviors are going to be rational or that people will even necessarily feel better about themselves.
In sum, cognitive behavioral therapy is a collection of therapies, all of which assume that people’s behaviors and their feelings are influenced by the way they think about events. Events don’t cause us to believe or think or feel or act in a certain way. Rather, it’s the perception of those events. CBT is perhaps best known for its wide variety of techniques and interventions, some of which address cognitive, some of which address affective, and yet others draw from behavioral therapy to address behaviors. Finally, cognitive behavioral therapy contributes a lot to culturally competent practice and although it has strengths and limitations, it is currently the treatment intervention (or series of interventions) they have that have the most evidence base to support their efficacy.
[47:11: END]
References
Bandura, A. (1977). Social learning theory. Englewood Cliffs, N.J.: Prentice-Hall.
Burke, J. F. (1989). Contemporary approaches to psychotherapy & counseling: The self-regulation and maturity model. Belmont, CA: Wadsworth Press.
Burns, D. D. (1999). Feeling good: The new mood therapy (Rev. ed). New York: Avon.
Corey, G. (2005). Theory and practice of counseling and psychotherapy (7th ed). Belmont, CA: Wadsworth/Thomson.
Dattilio, F. M., & Goldfried, M. R. (1998). Case studies in couple and family therapy: Systemic and cognitive perspectives. New York: Guilford Press.
Freeman, A., Pretzer, J., Fleming, B., & Simon, K. M. (2004). Clinical applications of cognitive therapy (2nd ed. ed.). New York: Kluwer Academic/Plenum Publishers.
Rudd, M. D., Joiner, T. E., & Rajab, M. H. (2001). Treating suicidal behavior: An effective, time-limited approach. New York: Guilford Press.
Rychlak, J. F. (1981). Introduction to personality and psychotherapy (2nd ed.). Boston: Houghton Mifflin Company.
Tomb, M., & Hunter, L. (2006). Effective interventions for students with obsessive-compulsive disorder. In C. Franklin, M. B. Harris & P. Allen-Meares (Eds.), The school services sourcebook: A guide for school-based professionals (pp. 89-109). New York: Oxford University Press.
Vonk, M. E., & Early, T. J. (2002). Cognitive-behavioral therapy. In A. R. Roberts & G. J. Greene (Eds.), Social workers' desk reference (pp. 116-120). New York: Oxford University Press.
APA (6th ed) citation for this podcast:
Singer, J. B. (Host). (2008, March 19). Cognitive-behavioral therapy [Episode 14]. Social Work Podcast. Podcast retrieved Month Day, Year, from http://socialworkpodcast.com/2007/03/cognitive-behavioral-therapy-cbt.html

5 comments:
CBT can help you to change how you think ("Cognitive") and what you do ("Behaviour)". These changes can help you to feel better. Unlike some of the other talking treatments, it focuses on the "here and now" problems and difficulties. Instead of focussing on the causes of your distress or symptoms in the past, it looks for ways to improve your state of mind now.
It has been found to be helpful in Anxiety, Depression, Panic, Agoraphobia and other phobias, Social phobia, Bulimia, Obsessive compulsive disorder, Post traumatic stress disorder and Schizophrenia.
http://de-adiction.blogspot.com
This leaflet is for anyone who wants to know more about Cognitive Behavioural Therapy (CBT). It discusses how it works, why it is used, its effects, side-effects, and alternative treatments. If you can't find what you want here, there are sources of further information at the end of this leaflet.
http://addiction-of.blogspot.com
http://abuse-of.blogspot.com
The cognitive behavioral therapies are helpful in the treatment of depression and hypertension. It assists those who are pessimist in life and dont see the positive part of the things. The therapy changes the point of view and offers them the optimistic life. The therapy supports a lot in maintaining the good relationship between the drug addicted patients and their family as well as with the society.
http://www.edrugrehabs.com/
Great topic, you covered some really good information. Thanks for this podcast Jonathon.
CBT concentrates on now, nearly always at the complete exclusion of all formative experiences. It does not ask why, and why is always paramount in the mind. The problem is that this methods makes roughly about as much sense as ignoring a person's physical medical history when treating them. The way CBT is usually done is similar to telling a person with a broken leg to "work as a team" with the therapist to investigate the patients irrational feelings about their leg.
The trouble is their feelings may very well not be irrational. That is an assumption, not a given.
Many issues due cause feedback into the physical function and structure of the brain itself. PTSD and anxiety issues produce changes to the amygdala, which is a form of organ failure. Using CBT to address that sort of damage is outright insulting to the patient (and their experiences and emotional pain) and to the intelligence of anyone who really DOES understand how neuroplasticity works. Challenging the patients stress responses can actually cause further damage.
You may as well tell our theoretical patient with the broken leg their troubles will go away if they just abandon the idea that there is something wrong with their leg, and take up long distance running.
Post a Comment